What is an Orthopedic Implants Plates and How Are They Used?
Orthopedic implants plates are crucial in modern surgical practices. These devices support bone healing after fractures or surgeries. According to the Global Orthopedic Implants Market Report, the market is projected to reach $66.9 billion by 2025. This growth reflects the rising incidence of orthopedic disorders and an aging population.
Orthopedic implants plates come in various shapes and materials, ensuring optimal fit and support. They play a vital role in stabilizing bone fragments and promoting recovery. The proper use of these plates can significantly reduce recovery time. However, not all surgeries achieve the desired outcomes. Surgical technique, patient health, and implant type can impact success.
Despite advancements, complications can occur. The risk of infection or non-union persists in some procedures. Healthcare professionals must choose wisely, guided by their experience and current research. Understanding these complexities can enhance patient outcomes. Hence, the knowledge of orthopedic implants plates is more than technical—it’s vital for improving lives.

What Are Orthopedic Implant Plates and Their Functions in Surgery?
Orthopedic implant plates play a crucial role in surgical procedures aimed at repairing bones. These plates are typically made from biocompatible materials, ensuring they can integrate smoothly with the body. Surgeons use them to stabilize fractured bones, providing the necessary support during the healing process. Their design allows for attachment to the bone with screws, which helps achieve an optimal alignment. While effective, challenges can arise. Misalignment during placement can lead to complications.
The functions of orthopedic implant plates extend beyond just stabilization. They can aid in the reconstruction of bone integrity. In complex cases, surgeons must consider the plate's size and shape to match the specific anatomy of the patient. This often requires a tailored approach. Surgeons may face difficulties when implanting these devices, as poor selection can affect patient outcomes.
In specialized procedures, plates may be combined with other methods. This multidimensional strategy can enhance healing. Nonetheless, the surgeon's expertise remains critical. Continuous education and experience are vital for mastering these techniques. Balancing innovation with practical knowledge is key in this field.
Usage and Types of Orthopedic Implant Plates in Surgery
Types of Orthopedic Implant Plates: Overview and Applications
Orthopedic implant plates are essential tools in modern orthopedic surgery. They serve to stabilize and support fractured bones. Various types of implant plates exist, each designed for specific applications. Common types include dynamic compression plates, locking plates, and recon plates. Locked plates provide enhanced stability, particularly in complex fractures. Their design allows for improved bone healing.
The application of these plates is broad. In trauma cases, they help secure bone fragments tightly. A study published in the Journal of Orthopedic Research noted that over 70% of surgeons preferred locking plates for challenges posed by osteoporotic bones. Biomechanical properties are vital here. Plates must withstand significant loads during the healing process. Furthermore, some cases reveal that improper plate placement can result in complications, highlighting the need for surgical precision.
In reconstructive surgeries, plates facilitate bone alignment. They also play a role in joint repair. Reports indicate a rise in their usage, especially for elbow and knee reconstructions. Despite technological advancements, issues still arise. Plates can sometimes lead to patient discomfort or infection. Overall, orthopedic plates remain a cornerstone of surgical intervention, offering both stability and support.
Materials Used in Orthopedic Implant Plates: Strength and Biocompatibility
Orthopedic implant plates play a crucial role in bone healing and stabilization. These plates are often used in surgical procedures to align and support fractured bones. The materials selected for these implants significantly impact their effectiveness. Strength and biocompatibility are key factors that healthcare professionals consider during their selection process.
Common materials used in orthopedic implant plates include stainless steel and titanium. Stainless steel offers excellent strength and durability, making it suitable for load-bearing applications. However, its lack of biocompatibility can lead to undesirable responses in some patients. In contrast, titanium is lighter and more biocompatible, reducing the risk of complications. Yet, it may not provide the same level of strength as stainless steel in high-stress environments.
The choice of materials is a reflection of ongoing advances in orthopedic medicine. Understanding the properties of each material helps in making informed decisions during surgery. It's essential to balance strength with biocompatibility. Some patients may experience discomfort from specific materials. This reality underscores the need for continuous evaluation and research in implant design to optimize patient outcomes.
What is an Orthopedic Implants Plates and How Are They Used?
| Material | Strength (MPa) | Biocompatibility | Common Uses |
|---|---|---|---|
| Titanium | 130-150 | Excellent | Fracture fixation, joint replacements |
| Stainless Steel | 200-220 | Good | Bone plates, screws |
| Cobalt-Chromium | 350-500 | Excellent | Hip and knee implants |
| Polyetheretherketone (PEEK) | 80-100 | Good | Spinal implants, plates |
| Bioactive Glass | 50-70 | Very Good | Bone regeneration applications |
Surgical Techniques for Applying Orthopedic Implant Plates in Fracture Repair
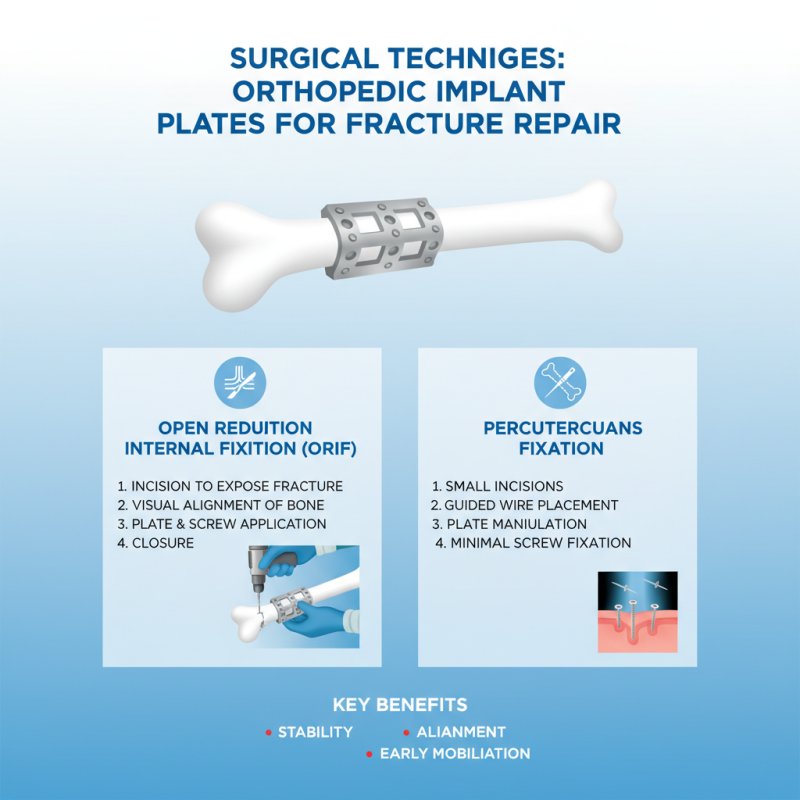
Orthopedic implant plates play a crucial role in fracture repair. These plates provide stability to broken bones, aligning them for proper healing. Surgical techniques for applying these plates require precision and skill. Surgeons often use various methods such as open reduction internal fixation (ORIF) or percutaneous fixation, depending on the fracture type.
In ORIF, the surgeon exposes the fracture site, realigns the bones, and affixes the plate with screws. This method allows direct visualization. Surgical studies indicate that ORIF significantly reduces complication rates. However, it requires careful planning and knowledge of the patient's anatomy. This complexity makes training essential for all medical professionals involved.
Tip: Ensure patients understand the recovery process after surgery. Educating them improves compliance and outcomes. Compression, immobilization, and proper nutrition are vital for successful healing.
The percutaneous technique is less invasive. Surgeons make small incisions and guide instruments to place the plate indirectly. This method can minimize soft tissue damage. However, it also presents challenges in achieving alignment. This technique may not be suitable for all fractures. Moreover, the risk of infection still exists.
Tip: Regular follow-up appointments are crucial. They help monitor healing and adjust treatments as necessary. Addressing any complications early can lead to better results during recovery.
Post-Operative Care and the Role of Orthopedic Implant Plates in Recovery
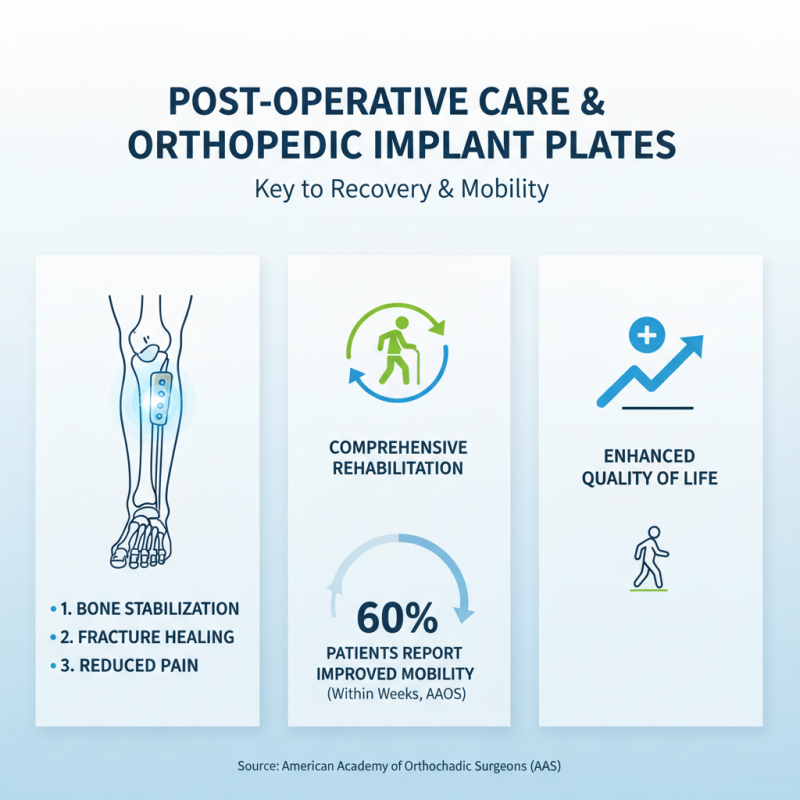
Orthopedic implant plates are crucial in post-operative care. These devices stabilize fractured bones, allowing proper healing. Post-surgery, patients often require comprehensive rehabilitation. According to the American Academy of Orthopaedic Surgeons, 60% of patients report improved mobility within weeks after using these implants.
Careful monitoring of the surgical site is essential. Infections or complications can arise, impacting recovery. A study published in the Journal of Orthopaedic Research emphasized that timely follow-up can reduce post-operative complications by up to 30%. Health professionals stress the importance of adhering to prescribed physical therapy routines. Proper guidance enhances recovery outcomes and minimizes risks.
Patients often face challenges during their recovery journey. Pain management and mobility issues can hinder progress. Research indicates that 20% of patients feel discouraged during rehab. Open communication with healthcare providers can address these concerns, fostering a better healing environment. Continued education about recovery and realistic expectations plays a key role in patient morale.
Related Posts
-

Top 10 Best Orthopedic Implants Plates You Should Know?
-

10 Essential Tips for Choosing Orthopedic Implants Screws
-

What are Orthopedic Implants Instruments and Their Uses?
-
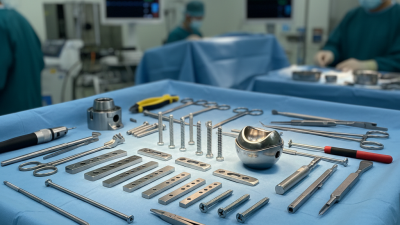
What is Orthopedic Surgical Items and Their Importance in Medicine?
-
How to Use Bone Plates for Optimal Healing and Recovery?
-
2026 Best Orthopedic Locking Screws for Enhanced Surgical Outcomes?
