Why is the Locking Plate Essential for Modern Orthopedic Surgery?
The locking plate has revolutionized modern orthopedic surgery. It provides unmatched stability in fracture fixation. Surgeons rely on its innovative design to enhance bone healing. Traditional plates often lead to complications due to their dependency on soft tissue for stability. In contrast, a locking plate connects directly to the bone. This connection significantly reduces the risk of implant loosening.
The precision of the locking mechanism ensures consistent results. It allows for angular stability, giving surgeons better control during procedures. In cases with complex fractures, the benefits of a locking plate shine. They permit less invasive techniques, minimizing damage to surrounding tissues. Patients experience shorter recovery times and improved outcomes.
Despite these advancements, challenges remain. Surgeons must carefully evaluate each case to determine the best approach. Not every fracture will benefit from a locking plate. This decision requires significant expertise and experience. The evolution of orthopedic surgery continues, driven by the need for more effective solutions. The locking plate is a prime example of this progress.
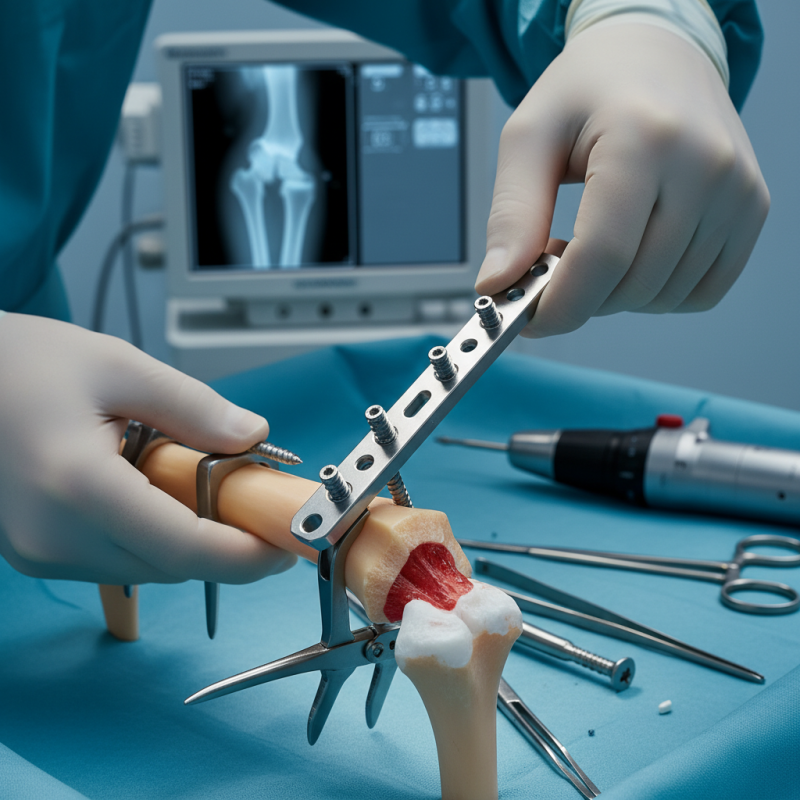
The Concept of Locking Plates in Orthopedic Surgery
Locking plates have revolutionized orthopedic surgery by providing enhanced stability and fixation. These innovative devices feature locking screws that secure the plate to the bone. Unlike traditional plates, locking plates allow for angular stability, making them suitable for complex fractures and osteoporotic bones. According to a study published in the Journal of Orthopaedic Trauma, the use of locking plates has led to a 30% reduction in non-union rates among patients.
The design of locking plates makes them particularly effective in challenging surgical scenarios. Their ability to maintain the appropriate contour and alignment of fractured bones is crucial. A report from the American Academy of Orthopaedic Surgeons highlights that 85% of orthopedic surgeons report increased confidence when using locking plates in surgery. However, challenges remain, such as implant complexity and potential complications. Surgeons must carefully evaluate each case to ensure the appropriate selection of implants.
Despite their advantages, locking plates also present a learning curve. Surgeons must develop a thorough understanding of their mechanics. Proper placement and technique can be critical in achieving successful outcomes. Continual education and training are vital to mastering these advanced tools in orthopedic surgery. As the field evolves, the role of locking plates is increasingly prominent, yet reflection on their limitations remains important for improving surgical practice.
Why is the Locking Plate Essential for Modern Orthopedic Surgery? - The Concept of Locking Plates in Orthopedic Surgery
| Feature | Description | Benefits | Applications |
|---|---|---|---|
| Stability | Provides biomechanical stability to fractured bones by locking screws into place. | Enhanced healing and reduced risk of non-union. | Long bone fractures, complex joint fractures. |
| Versatility | Compatible with various fracture types and locations. | Applicable in multiple surgical scenarios. | Trauma surgery, orthopedic surgery, pediatrics. |
| Ease of Use | Designed with user-friendly features for efficient application during surgery. | Reduces surgical time and complications. | Elective and emergency surgeries. |
| Innovation | Incorporates advanced materials and design technologies. | Improves patient outcomes and minimizes complications. | Fractures requiring surgical intervention, osteosynthesis. |
Historical Development of Locking Plate Technology
The evolution of locking plate technology is a remarkable journey. In the early 2000s, locking plates gained traction as a revolutionary tool in orthopedic surgery. Prior to that, surgeons relied heavily on traditional plating systems. These conventional methods often led to complications, such as malalignment and plate cut-out. Studies indicated that nearly 30% of fractures treated with standard plates had unsatisfactory results.
The introduction of locking plates changed the game. They allow for fixed-angle stability, which improves fracture healing and patient outcomes. Research shows that locking plates can reduce revision surgeries by up to 40%. This improvement is significant, considering that about 20% of orthopedic surgeries face complications requiring additional intervention. Surgeons have the ability to provide more stable constructs, especially in osteoporotic bones. The development of these plates marked a shift towards more reliable and effective surgical techniques.
However, reliance on locking plates raises questions. While they enhance surgical outcomes, their expense can strain healthcare budgets. The high cost of materials often leads to a disparity in resource availability. In some regions, access to advanced locking plate technology is limited. This raises ethical considerations about equitable care. The journey of locking plate technology reflects both tremendous progress and a need for ongoing reflection in modern orthopedic practices.
Advantages of Locking Plates Over Traditional Fixation Methods
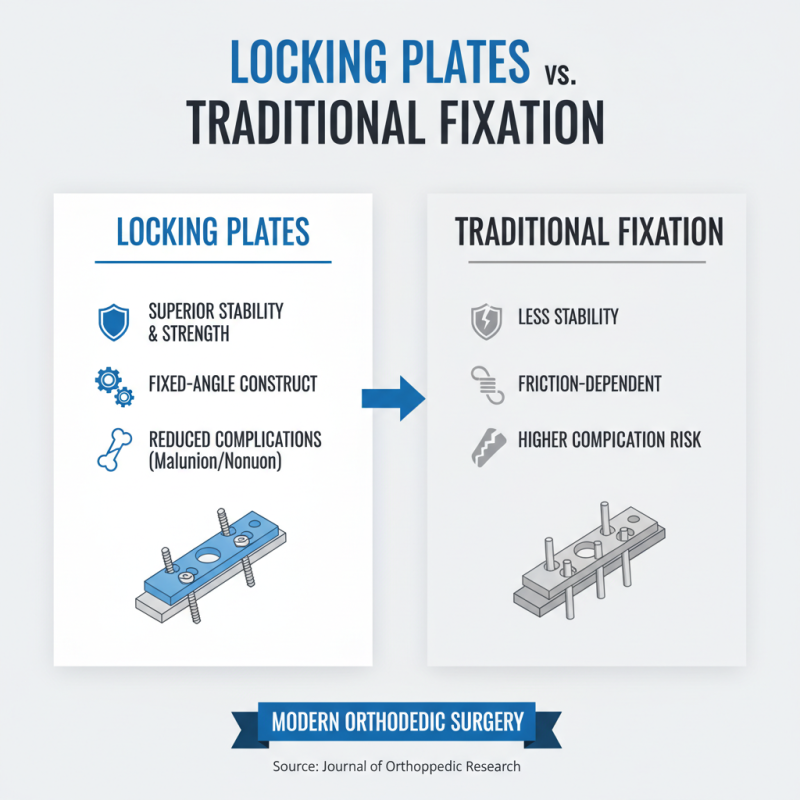
Locking plates have become a cornerstone in modern orthopedic surgery due to their numerous advantages over traditional fixation methods. A report from the Journal of Orthopedic Research indicates that locking plates provide superior stability in complex fractures. They are designed to maintain bone alignment even under stress, reducing the risk of malunion and nonunion. This strength is crucial in multi-fragmentary fractures where precise alignment is vital for recovery. Locking mechanisms enhance stability by creating a fixed-angle construct, which is less reliant on bone quality.
Moreover, data shows that surgeries using locking plates can reduce operation time by up to 30%. Faster surgical procedures translate to lower infection rates and improved patient outcomes. Despite these advantages, some surgeons remain cautious. Concerns about the rigidity of locking plates can lead to apprehension for certain patients who need controlled mobility during healing. Additionally, the learning curve for implementing these new techniques may deter some practitioners, highlighting the need for ongoing training. While locking plates are not without their challenges, the benefits in ensuring reliable fixation and better recovery outcomes are significant.
Applications of Locking Plates in Various Orthopedic Procedures
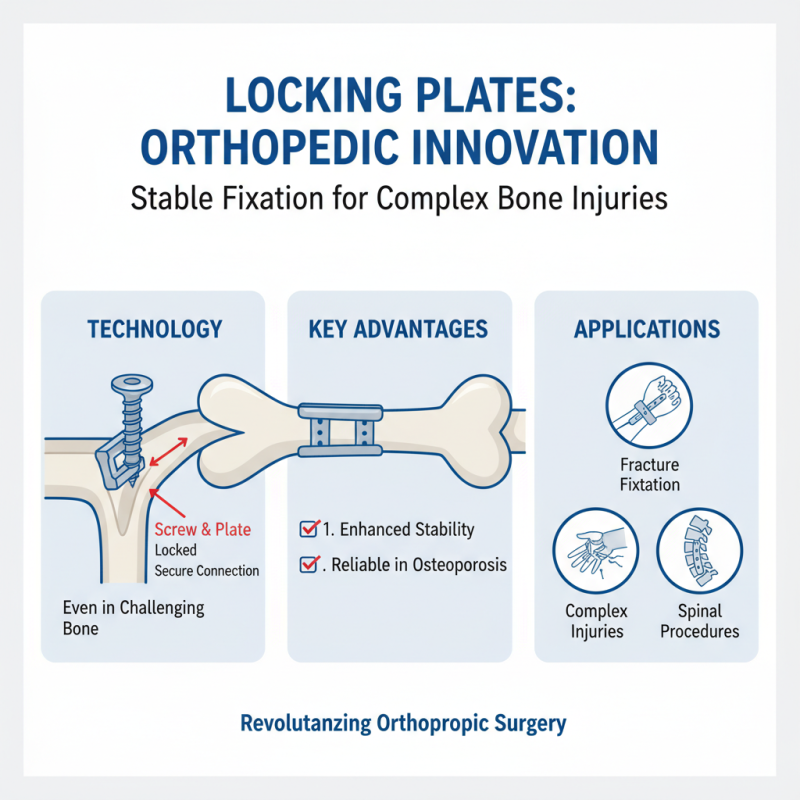
Locking plates have revolutionized modern orthopedic surgery. They provide stable fixation for fractures and complex injuries. Using locking technology, these plates maintain a secure connection between the screw and plate, even in challenging bone conditions. Surgeons find this particularly helpful in cases of osteoporosis, where traditional methods may fail.
Applications of locking plates are broad. They are commonly used in the fixation of fractures in the lower extremities, including the tibia and femur. In pediatric cases, locking plates aid in the treatment of growth plate injuries. This technology allows for proper alignment and healing. However, surgeons must carefully assess each patient. In some cases, the use of locking plates can lead to complications, such as implant failure or poor bone healing.
Surgeons often reflect on the learning curve associated with these devices. Not all scenarios are ideal for locking plates. In certain fractures, traditional non-locking plates may still perform better. Continuous education and hands-on experience are vital. Understanding the specific needs of each patient can significantly impact outcomes. Thus, the choice between locking and non-locking options should always be made wisely.
Future Trends and Innovations in Locking Plate Design and Usage
The evolution of locking plate technology significantly impacts orthopedic surgery. Recent data indicate that the global locking plate market is projected to reach approximately $3.5 billion by 2027. This growth highlights the increasing reliance on innovative designs for enhanced patient outcomes.
Current trends include advancements in material science, resulting in lighter and stronger locking plates. Researchers are focusing on bioresorbable materials, reducing the need for plate removal surgeries. A study from the Journal of Orthopaedic Research revealed that these materials can improve healing times and reduce complications. However, more research is needed to address concerns regarding their long-term stability and performance.
Tips: When considering locking plates, surgeons should assess each patient’s unique needs. Collaborating with biomaterial experts can improve device selection. Stay updated on emerging technologies and clinical trials.
Reflections on locking plate designs reveal challenges. While these plates offer rigidity and stability, they may also lead to complications such as stress shielding. Balancing stability and biological healing is key to progress. Orthopedic professionals must remain vigilant about these trade-offs as they embrace future innovations.
Usage of Locking Plates in Orthopedic Surgery
Related Posts
-
How to Choose the Right Surgery Instruments for Your Medical Practice?
-
Why Are Bone Screws Essential in Modern Orthopedic Surgery?
-
Top 10 Orthopedic Locking Screws You Should Know About?
-
What is Orthopedic Surgical Items and Their Importance in Medicine?
-
2026 Best Orthopedic Surgical Instruments for Precision and Efficiency?
-
What Are Locking Screws and Their Top Applications?
