10 Essential Tips for Choosing Orthopedic Bone Screws Efficiently
When selecting orthopedic bone screws, the decision carries significant weight in surgical outcomes. Dr. James Caldwell, a prominent orthopedic surgeon, once noted, “Choosing the right screw can mean the difference between quick recovery and prolonged pain.” This highlights the importance of careful consideration in this critical aspect of orthopedic procedures.
Orthopedic bone screws come in various sizes and materials, making the selection process complex. Surgeons must assess factors such as compatibility with bone type and the nature of the injury. An inappropriate choice can lead to complications, including inadequate stabilization or delayed healing.
Moreover, professionals must confront the reality that not all brands are equally reliable. Anecdotes in the field reveal instances where low-quality screws failed, resulting in additional surgeries. Therefore, understanding the nuances of orthopedic bone screws is essential. Making informed choices is vital for patient safety and recovery, calling for a deeper analysis of available options in this specialized market.

Understanding the Role of Orthopedic Bone Screws in Surgery
Orthopedic bone screws play a critical role in surgical procedures. They are used to stabilize and support fractured bones. These screws provide a reliable method for achieving bone union, essential for recovery. Each surgery presents unique challenges, and choosing the right screw is crucial. Factors such as the type of fracture and the bone's condition significantly affect decision-making. Surgeons must often consider both strength and flexibility when selecting screws.
Many surgeons have faced difficulties in understanding the range of available options. The sheer variety of orthopedic screws can be overwhelming. Size, length, and material are just a few considerations. Some surgeons may overlook the importance of matching screws to patient-specific needs. This error can lead to complications during recovery. It's essential for healthcare professionals to continuously educate themselves on the latest advancements in screw technology. Reflecting on past surgical outcomes can provide valuable insights for future procedures.
Key Factors to Consider When Selecting Bone Screws
Selecting orthopedic bone screws requires careful consideration of several factors. The material of the screws is paramount. Common options include titanium and stainless steel. Each has unique properties affecting biocompatibility and strength. For instance, titanium is lightweight and resistant to corrosion, while stainless steel is often more affordable but may face issues with long-term wear.
Next, the screw's size and thread type matter significantly. Larger screws may provide greater stability, but they can also damage surrounding tissues if not chosen correctly. Fine threads offer better fixation in softer bone. The screw length can affect the impact on bone healing, so precise measurement is crucial. Additionally, the design of the screw should align with the intended application, whether it’s for fracture fixation or spinal surgery.
Lastly, consider the ease of removal when necessary. Some screws, especially those used in temporary applications, should be easily extractable. However, that may not be the case with all screws, necessitating thoughtful planning during selection. It’s essential to balance the need for durability with the possibility of future adjustments. Each decision impacts patient outcomes, requiring a constant reflection on the choices made during the selection process.
Material Options for Bone Screws: Pros and Cons
When selecting bone screws, material choices play a crucial role.
Stainless steel is commonly used.
It offers strength and corrosion resistance. However, it may cause allergic reactions in some patients.
This can complicate recovery and lead to infections.
Titanium is another option. It's lighter and has excellent biocompatibility.
Many surgeons prefer it for its reduced risk of complications. Yet, titanium screws can be more expensive.
This can strain a hospital’s budget. Composite materials are emerging as alternatives.
They are bioabsorbable, meaning they can dissolve in the body over time.
On the downside, their mechanical stability may vary. It's essential to evaluate the specific needs of each patient and the surgical procedure.
Choosing the right material is not always straightforward. There are trade-offs with each option.
Surgeons need to think about the patient's history,
activity level, and long-term outcomes. The pressure to use high-quality materials can sometimes lead to hasty decisions.
Balancing cost, effectiveness, and patient safety is crucial.
A thoughtful approach may involve discussing with colleagues and considering past experiences.
Sizing and Dimensions: Importance in Surgical Applications
Choosing the right orthopedic bone screws is essential for successful surgical outcomes. Sizing and dimensions play a critical role in this selection process. The screws must fit precisely into the intended bone structure. Mismatched sizes can lead to complications during surgery. A well-sized screw provides stability and promotes healing.
When assessing screw dimensions, consider the bone anatomy. Bones vary greatly among patients. A standard size may not work for everyone. Surgeons should be aware of these variations. Inaccurate measurements can result in inadequate anchoring or excessive stress. This could lead to screw failure or prolonged healing times.
Surgeons often rely on preoperative imaging to determine appropriate sizes. However, this isn’t foolproof. Imaging can sometimes mislead due to underlying conditions. It's crucial to remain adaptable during surgery. Carrying a range of sizes can be beneficial. This way, adjustments can be made as needed. Every surgical situation is unique, and being prepared can significantly improve outcomes.
10 Essential Tips for Choosing Orthopedic Bone Screws Efficiently
This chart illustrates the key characteristics to consider when selecting orthopedic bone screws, highlighting their respective dimensions and types. Understanding these parameters is critical for ensuring optimal surgical outcomes.
Evaluating Cost-Effectiveness and Quality of Bone Screws
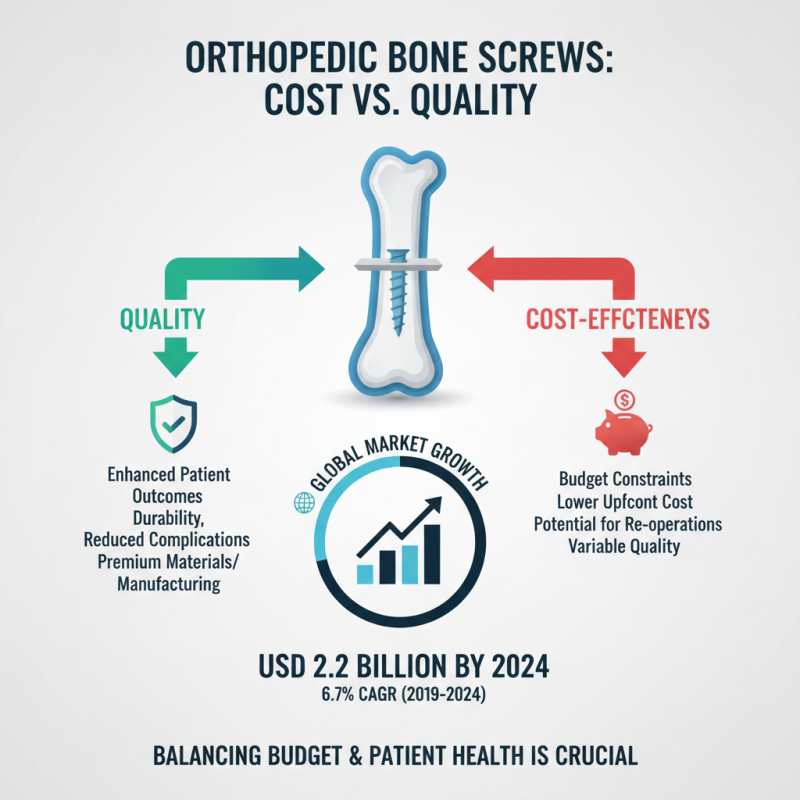
When it comes to choosing orthopedic bone screws, evaluating cost-effectiveness and quality is crucial. The global orthopedic screw market is expected to reach USD 2.2 billion by 2024, growing at a CAGR of 6.7% from 2019 to 2024. This growth indicates increasing demand for high-quality orthopedic solutions. However, not all bone screws are created equal. Often, surgeons and hospitals face budget constraints, leading them to select lower-cost options that may compromise quality.
One study found that around 30% of lower-cost screws failed in clinical applications due to material defects. In contrast, high-quality screws exhibit significantly better performance, with a failure rate of less than 5%. This data underscores the importance of choosing reliable suppliers and understanding the materials used in production. For example, screws made of titanium or stainless steel typically offer superior strength and biocompatibility. However, these advantages come at a higher initial cost, which can be a barrier for some medical facilities.
Evaluating all aspects of bone screws is essential. Consider long-term costs, not just the purchase price. A higher-quality screw may lead to better patient outcomes, reducing the need for revisions and additional procedures. However, hospitals must assess their budgets carefully. They must find a balance between cost and quality. An informed choice could improve both patient care and operational efficiency.
Related Posts
-
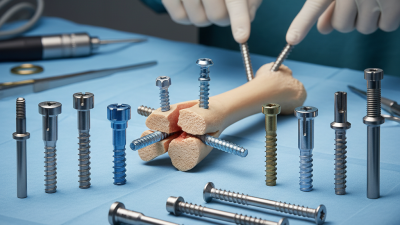
Top 10 Best Orthopedic Bone Screws for Effective Fracture Healing?
-

Orthopedic Plates and Screws Tips for Better Healing
-

Top 7 Tips for Choosing Orthopedic Surgical Plates for Your Needs
-

How to Choose the Right Orthopedic Surgical Plates for Your Surgery?
-
Why Are Bone Screws Essential in Modern Orthopedic Surgery?
-
Top 10 Orthopedic Locking Screws You Should Know About?
