How to Choose the Right Orthopedic Surgical Plates for Your Surgery?
Choosing the right orthopedic surgical plates is crucial for successful surgeries. Dr. John Thompson, a leading orthopedic surgeon, once said, "The choice of surgical plate can determine the outcome of the procedure." These plates stabilize fractures and bear the load during healing.
When selecting orthopedic surgical plates, various factors come into play. Not all plates are created equal. They come in different materials, shapes, and sizes. Understanding these differences is essential. For instance, titanium plates are strong yet lightweight, while stainless steel offers durability. Surgeons must weigh the benefits and drawbacks of each option.
It's important to consider the patient's unique anatomy. Not every plate fits every body. Surgeons should reflect on past surgeries and outcomes. What worked well in one case may fail in another. When in doubt, consulting with colleagues adds valuable insights. This thoughtful approach can make a significant difference in surgical success.
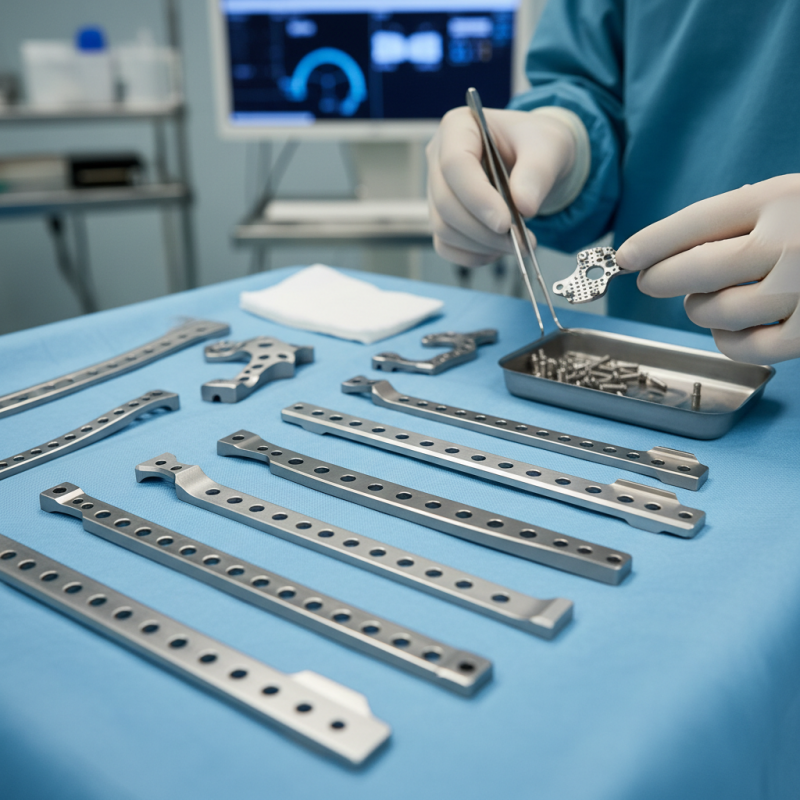
Understanding Orthopedic Surgical Plates: Types and Uses
Orthopedic surgical plates are vital in bone fixation and stabilization. They come in various types, each designed for specific surgical needs. There are locking plates, dynamic compression plates, and$row plates, among others. Each type offers unique benefits. For instance, locking plates enhance stability for complex fractures, while compression plates are ideal for promoting healing in simple fractures.
In a recent report by the Orthopedic Surgeons Society, nearly 30% of surgical complications stem from improper plate selection. This statistic underscores the importance of understanding the anatomy and mechanics involved. Surgeons must assess the type of fracture, bone quality, and expected load. Inadequate plate support can hinder recovery or lead to additional surgeries.
Surgeons sometimes struggle with choices. The learning curve involves evaluating patient-specific factors, such as age and activity level. A plate suitable for one patient may not suit another. Clinical experience and data drive these decisions. Reflection on past surgical outcomes can help refine future choices. Adapting to new evidence can be challenging, but it’s essential for patient safety.
Usage of Different Orthopedic Surgical Plates by Type
Factors to Consider When Selecting Orthopedic Surgical Plates
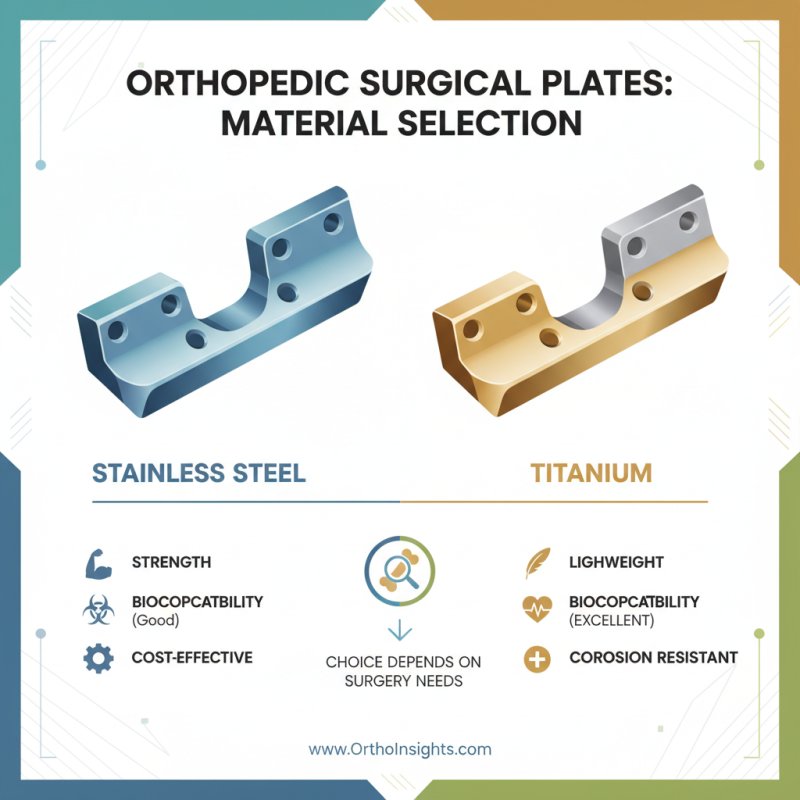
When selecting orthopedic surgical plates, several key factors come into play. Material composition is crucial. Stainless steel and titanium are common options. Each has unique benefits, affecting strength and biocompatibility. The choice depends on the specific needs of the surgery.
Plate size and shape are also essential. It must fit the anatomy of the patient accurately. An improper fit can lead to complications. Additionally, consider the plate's screw type and placement. This decision impacts stability and healing time. Sometimes the available options seem overwhelming.
It’s important to partner with an experienced surgical team. Their insights can guide your decisions. However, even seasoned professionals can face challenges. Misjudgments can lead to suboptimal outcomes. Regular reviews and feedback are necessary for improvement. It’s a continuous learning process in the operating room.
Evaluating Plate Materials and Their Properties
When choosing orthopedic surgical plates, evaluating the material is crucial. Common materials include titanium, stainless steel, and polyamide. Titanium is lightweight and highly resistant to corrosion. Stainless steel provides excellent strength but can be heavier. Polyamide, while less common, offers flexibility. Each material has its unique properties affecting their performance.
Research indicates that tensile strength varies considerably among these materials. For instance, titanium boasts a tensile strength of about 900 MPa, while stainless steel ranges from 400 to 600 MPa. The choice of material can directly influence healing time and surgical outcomes. Yet, the complexity of bone biology means that even the best material choice may not guarantee success.
Surgeons often face challenges when selecting the appropriate plate. The surgical setting and patient specifics can complicate decisions. For example, osteoporotic patients may require different plate designs than younger, healthier individuals. There's no one-size-fits-all solution. Continuous research is essential to improve these choices and adapt to patient needs.
Assessing Patient-Specific Needs for Plate Selection
Choosing the right orthopedic surgical plates is critical for successful outcomes. Every patient's anatomy and needs vary significantly. According to a study published in the Journal of Orthopedic Research, around 30% of surgical failures are attributed to improper plate selection. This statistic emphasizes the necessity of first assessing each patient's unique requirements.
Patient-specific factors include bone density, age, and underlying medical conditions. For instance, an elder patient with osteoporosis will need a different plate compared to a younger athlete with healthy bones. The American Academy of Orthopaedic Surgeons suggests that customized solutions often yield better results. A biomechanical analysis shows that plates tailored to a patient's anatomy can enhance stability and promote quicker healing.
However, the process is not without its challenges. Surgeons must sometimes rely on pre-existing plates, which may not optimally fit the individual. This compromise can lead to complications like delayed union or non-union. Adapting to specific cases can also involve more intricate planning and collaboration among the surgical team, which might not always be feasible within time constraints. It’s essential to consider each element carefully, as small oversights can have significant impacts on patient recovery.
How to Choose the Right Orthopedic Surgical Plates for Your Surgery? - Assessing Patient-Specific Needs for Plate Selection
| Patient Age Group | Bone Condition | Plate Material | Plate Type | Recommended Size |
|---|---|---|---|---|
| Pediatric (0-12 years) | Healthy Bone | Titanium | Dynamic Compression Plate | Small (3-5 mm) |
| Adult (13-64 years) | Osteoporotic Bone | Stainless Steel | Locking Plate | Medium (5-8 mm) |
| Elderly (65+ years) | Fractured Bone | Bioactive Ceramic | Tension Band Plate | Large (8-10 mm) |
| Adult (13-64 years) | Healthy Bone | Titanium Alloy | Synthes Plate | Medium (5-8 mm) |
Consulting with Surgical Teams for Optimal Plate Choices
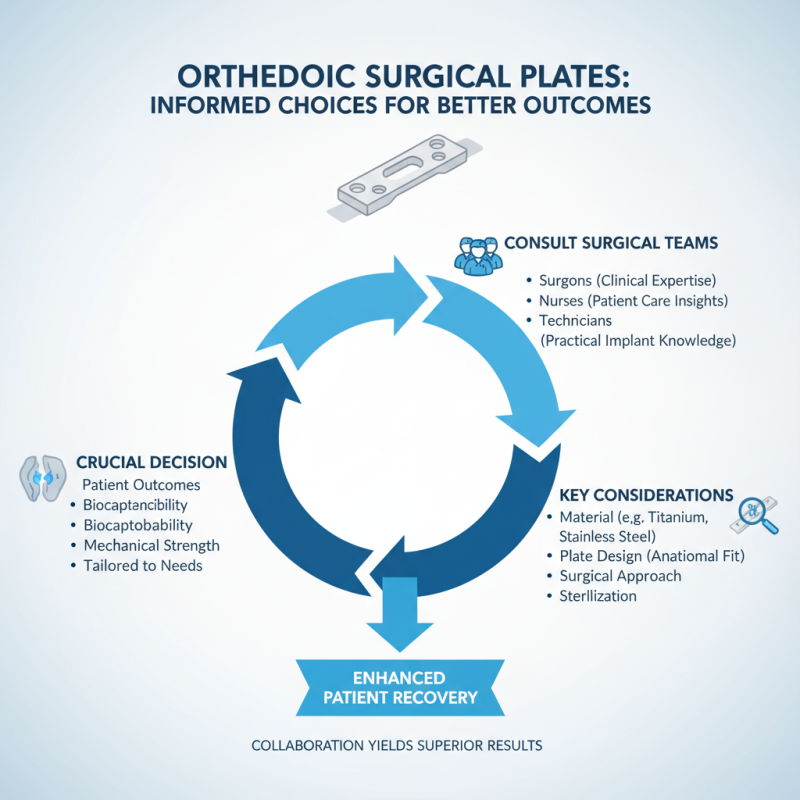
Choosing the right orthopedic surgical plates is crucial for patient outcomes. Before making a decision, consulting with surgical teams is essential. These teams consist of surgeons, nurses, and technicians who understand both the clinical and practical implications of different plate options. Their insights can help identify the best materials and designs tailored to specific surgical needs.
Research shows that approximately 35% of surgical complications arise from inadequate pre-surgical planning. Engaging surgical teams can significantly reduce this risk. These professionals often rely on data from clinical studies that reveal success rates of various plates. For instance, a recent study highlighted that titanium plates showed a 15% better integration rate compared to alternatives in specific procedures. Understanding these nuances of material selection can lead to more effective surgeries.
Moreover, communication during those discussions can uncover potential flaws. Even experienced teams can overlook the implications of certain choices. For instance, certain plates may not perform well in the presence of osteoporotic bone. A lack of attention to detail in these matters might lead to unexpected outcomes. Adjusting approaches based on team feedback can enhance surgical success. Emphasizing a collaborative environment ensures that all perspectives contribute to the final decision.
Related Posts
-

Top 7 Tips for Choosing Orthopedic Surgical Plates for Your Needs
-

Orthopedic Plates and Screws Tips for Better Healing
-

How to Choose the Best Implant Surgical Instruments for Your Practice?
-
2026 Best Orthopedic Surgical Instruments for Precision and Efficiency?
-
Top Surgical Instruments Tips for Beginners to Enhance Skills?
