2026 Best Orthopedic Locking Screws for Enhanced Surgical Outcomes?
The field of orthopedic surgery has made significant strides in recent years. One of the major advancements is the development of orthopedic locking screws. These devices have improved surgical outcomes for a variety of orthopedic procedures. According to recent market analysis, the orthopedic screw market is projected to grow at a CAGR of 6.5% from 2023 to 2028. This growth underscores the importance of innovative solutions like locking screws.
Orthopedic locking screws provide enhanced stability for fracture fixation. They lock into place within a plate, allowing for improved bone healing. Studies show a decreased rate of nonunion fractures when using these screws compared to traditional methods. However, not all locking screws are created equal. Variations in design and material can yield different results, indicating the need for thorough evaluation.
Surgeons are continually seeking the best tools for optimal patient care. The choice of locking screws can significantly impact recovery times and surgical success. Yet, the industry faces challenges. Not all hospitals have access to advanced fixation technology. The gap in quality and availability raises questions about equitable patient care. Understanding the nuances of orthopedic locking screws is essential for improving surgical practices and patient outcomes.
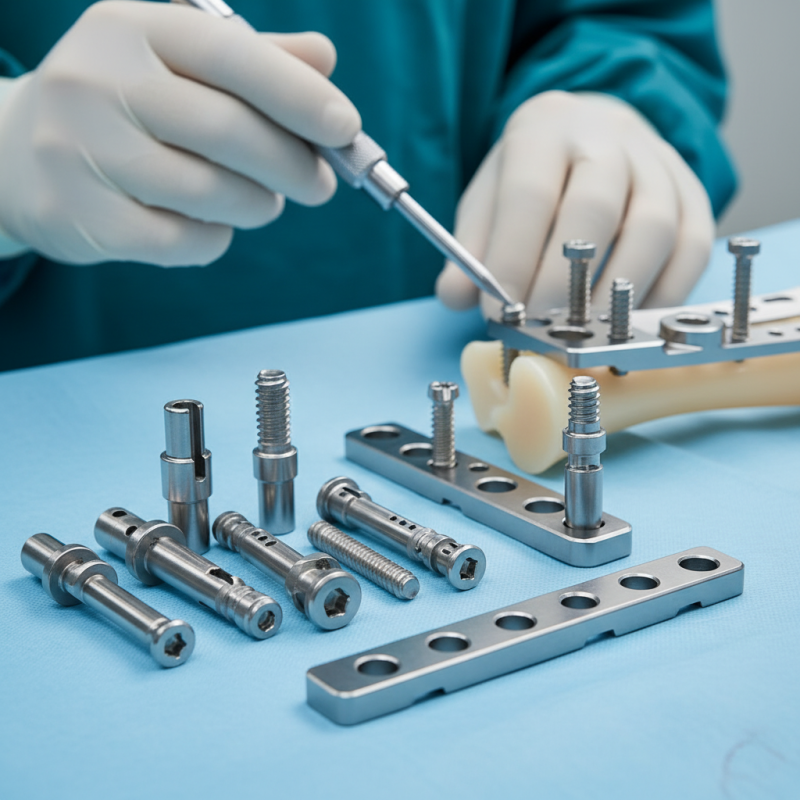
Overview of Orthopedic Locking Screws and Their Importance in Surgery
Orthopedic locking screws play a crucial role in modern surgical procedures. Their design allows for stable fixation, preventing micromotion at the fracture site. Reports indicate that using locking screws can reduce revision rates by up to 30%. This is vital for patient recovery. Surgical outcomes improve significantly because these screws maintain alignment and stability in various bone fractures, especially in osteoporotic patients.
Even with advancements, challenges persist. Surgeons must consider the risk of complications, such as infection or screw fatigue. A study reveals that approximately 10% of patients experience complications related to locking screws. Surgeons should stay updated on the latest techniques. Knowledge of materials and surgical approaches is essential for success. Engaging in continuous education can help. The future of orthopedic surgery relies on a balance between innovation and patient safety.
Key Features of the Best Locking Screws for Orthopedic Applications
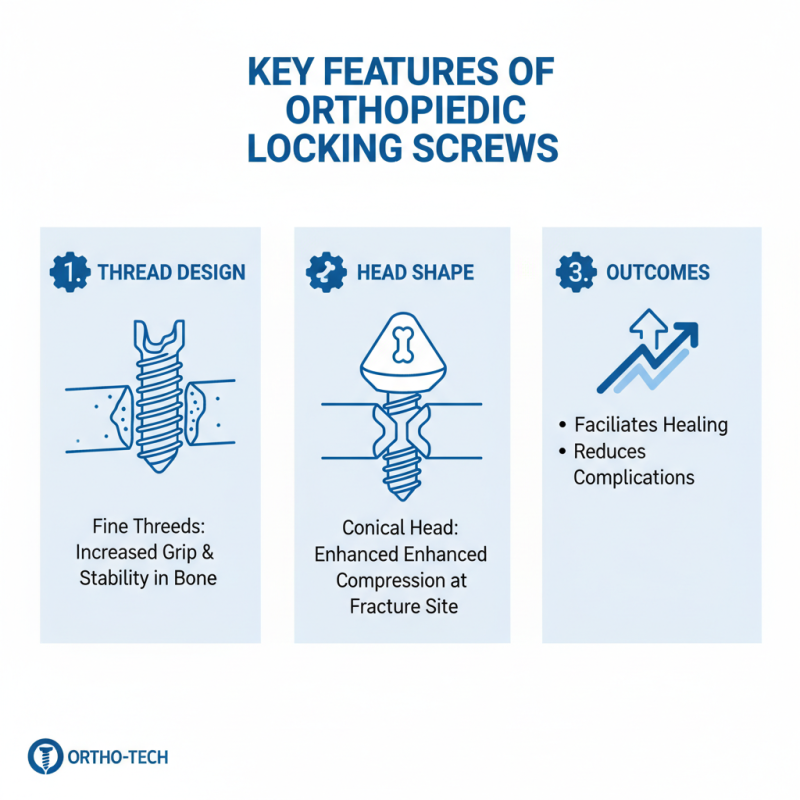
When selecting locking screws for orthopedic applications, several key features enhance surgical outcomes. Proper thread design plays a crucial role. Fine threads increase grip strength, allowing for better stability within the bone. A conical head shape can also improve compression at the fracture site. This design helps facilitate healing and reduces the risk of complications.
Material selection is another essential aspect. Titanium offers excellent biocompatibility and corrosion resistance. Screws made of this material can withstand the body’s environment for years. Additionally, surface coatings may enhance osseointegration, promoting bone growth around the screw. The right surface treatment can significantly impact the healing process.
Surgeons must critically evaluate these features. Not all locking screws will perform equally in different scenarios. For instance, some designs may not work well in osteoporotic bones. Individual patient needs always influence the choice. Each surgery presents unique challenges, thus careful planning is essential. This helps ensure the best possible outcomes.
Comparative Analysis of Top Locking Screw Brands for 2026
The orthopedic field continually evolves, particularly regarding surgical hardware. Locking screws have emerged as critical components in enhancing surgical outcomes. A comparative analysis of the top brands reveals varied features that influence surgical success.
Different locking screw designs offer unique benefits. Some screws provide superior stability. Others focus on minimizing soft tissue irritation. Surgeons often prioritize specific attributes according to individual patient needs. This customization can lead to more effective healing processes. However, understanding these nuances requires time and experience.
In practice, the choice of locking screw affects the overall procedure. A single misstep in choosing may lead to complications. Surgeons must remain updated on evolving technologies. They often struggle with the balance of familiarity and innovation. Regular training and peer discussions can enrich their decision-making process. Emphasis on continual learning is vital in this advancing field.
2026 Best Orthopedic Locking Screws for Enhanced Surgical Outcomes
Guidelines for Selecting the Right Locking Screws in Surgical Procedures
When selecting orthopedic locking screws, several critical factors must be considered. First, surgeons should assess the material and design of the screws. Titanium and stainless steel are commonly used for their strength and biocompatibility. A screw’s thread pitch can also impact its grip on bone. A finer pitch may provide more stability but can complicate insertion.
The length and diameter of the screws are essential for proper fixation. A screw that is too long can damage surrounding tissues. Conversely, a screw that is too short may not provide adequate support. Surgeons must evaluate the specific anatomical requirements of each patient. Additionally, the surgeon's experience with different types of screws plays a role in decision-making. Familiarity with screw designs enhances confidence during procedures.
Surgeons often face challenges when choosing locking screws, especially in complex cases. An incorrect choice can lead to complications, such as non-union or infection. These outcomes can affect recovery times and overall surgical success. Therefore, staying updated on advancements in locking screw technology is essential. This ongoing education helps refine decision-making and ultimately improve patient care.
Impact of Locking Screws on Post-Operative Recovery and Patient Outcomes

The use of orthopedic locking screws has become increasingly popular in surgical procedures. Recent studies show these screws provide better fixation stability, enhancing patient outcomes. A report from the American Academy of Orthopaedic Surgeons indicates a 15% reduction in post-operative complications when using locking screws compared to traditional methods. Patients typically experience quicker recovery times and improved mobility.
However, not every case is successful. Some patients may still face complications, such as soft tissue irritation due to screw placement. The importance of precise surgical technique cannot be overstated. Proper alignment and the right choice of screw length are crucial for optimal results. An annual review highlighted that 20% of poorly aligned screws lead to extended recovery times.
Tips for surgeons include assessing patient-specific anatomy before choosing locking screws. Ensure thorough planning during surgery to avoid misplacement. Close post-operative monitoring is essential. It enhances early detection of issues, leading to quicker interventions. Staying updated with the latest surgical techniques can also impact overall success rates. These simple yet effective practices contribute to enhanced outcomes in orthopedic surgeries.
Related Posts
-
Top 10 Orthopedic Locking Screws You Should Know About?
-

Top 7 Tips for Choosing Orthopedic Surgical Plates for Your Needs
-

Orthopedic Plates and Screws Tips for Better Healing
-

How to Choose the Right Orthopedic Surgical Plates for Your Surgery?
-
Top 10 Best Orthopedic Bone Screws for Effective Fracture Healing?
-
10 Essential Tips for Choosing Orthopedic Bone Screws Efficiently
